Health Care Monitoring of Mobile Patients
by Giuseppe Amato, Stefano Chessa, Fabrizio Conforti, Alberto Macerata and Carlo Marchesi
A joint activity between ISTI-CNR, IFC-CNR and the University of Florence addresses the problem of medical devices and data integration in health care. This article proposes a system for the remote monitoring of patients based on recent developments in networking and data management.
ICT has been employed in medicine and health care for many years now with great success. However, the upgrade of existing medical instruments and the design of new medical applications as a result of continuous advances in information technology must not lead to a neglect of the real needs of patients and physicians. In this respect, ICT has failed so far to fully respond to requirements related to integration and approach methodologies. Although significant progress has been made with respect to the creation of new medical instruments, the same effort has not been devoted to the integration of these instruments in operational information systems where all the devices can be integrated into a single framework of health-care resources. It should be observed that this aspect is particularly critical since different medical devices and hospital data bases using different protocols and/or data representations may be unable to interact automatically, thus failing to provide efficient diagnostic support.
|
In our opinion, a new scheme for cooperation between data, devices and systems is needed. As an example, let us take the scenario of a home care patient after hospitalization for cardiac infarction. Although such a patient should be guaranteed a good quality of life, he/she still needs to be in constant contact with an expert physician so that his/her cardiac activity (eg the heart rate and peripheral blood pressure), body temperature and breathing frequency can be continuously monitored. However, the health condition of a patient can only be partially evaluated through his vital signals and must be mediated and integrated by other signals and information coming both from personal characteristics (risk factors, degree of disease, age, sex, family history, psychological features, etc.) and from the environmental context (eg whether in bed or mobile, by him/herself or in company, at work or at home, the season and the temperature, etc.). The monitoring system should be able to provide a feedback to the patient as well as notifying his status to somebody else, such as a relative, the family doctor, or the hospital, depending on the degree of alert detected, and possibly adapting the level of service (ie the intensity of the monitoring activity).
The above scenario requires the integration of different medical devices, of environmental data acquired by sensors located near the patient, of patient data available from the electronic medical records stored by the hospital, and of hospital administrative information about admission/discharge of patients, and the management of financial data and health care resources. Although the current technologies offer the necessary means to support this kind of health care, in our opinion it should be possible to access and integrate all available health care resources offering a continuous, widespread, cooperative health care system and tools for personalized patient monitoring.
To achieve this, the current view of a medical instrument as a stand-alone device needs to be rethought; it should become a node in a medical network providing results and acquiring external data in order to update its internal knowledge in order to provide customized signal/data processing and patient-oriented answers.
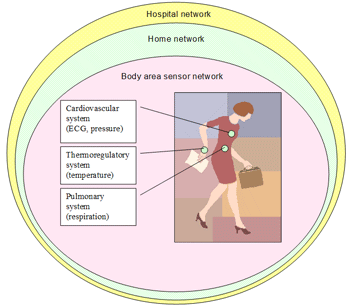
The medical network would be organized into layers with the patient at the centre. The inner layer which provides monitoring support is organized as a body area sensor network. This network, hosted by the patient, combines the patient's physiological data with information from the outer layers to support (basic) early diagnosis and produce (basic) alerts. The outer layer (for example the patient's domotic network) may include an environmental sensor network and one or more powerful nodes. Examples of such nodes could be an electrocardiograph offering diagnostic information or a PC receiving all the data and managing an advanced monitoring and alert detection service. This layer interacts with outermost layer (the hospital network) to exchange physiological data, alerts and patient-related data. Wireless connections should be used where possible to support mobility and adaptability at the various levels of the network.
Application scenarios of the type presented above give rise to several issues. The sensory devices constantly attached to the patient produce huge streams of physiological data which must be collected and related to environmental conditions. These sensors should be light and portable to reduce their impact on the patient's well-being (and thus must be constrained in terms of energy capacity). Consequently, the amount of information transmitted outside the network should be minimized in order to prolong its lifetime. Data is forwarded to and analysed by the hospital network only in certain (critical) cases; otherwise data is processed locally with the support of information from the patient's case history acquired from the hospital network.
For these reasons, we have developed a network and middleware layers for sensor networks, supporting the execution of queries originated by external controllers (such as a hospital network or a single physician locally connected via his notebook). The controller issues patient-specific queries which are optimized and distributed over the sensor network. These queries specify monitoring, data collection and/or processing tasks with different levels of intensity. They also define the flux of information between sensors.
Each sensor is thus assigned a sub-query defining the set of sensors providing the data streams necessary to execute the sub-query and the rules to combine such streams. At this level, communication between sensors is implicit since sensors only use operations to open, read or write local or remote data streams. At a lower level, opening a remote data stream implies that the data produced on a remote sensor should be routed and buffered on the local sensor.
The sensors manage streams via the middleware layer (called the stream system), which provides support for the management of local and remote data streams and for stream buffering and naming, and exploits the services of the network layer for routing.
The network layer provides support to the communication models used by the stream system (unicast and multicast). It defines a virtual coordinate system which assigns a coordinate to each sensor in the network and allows for efficient geographical routing.
The virtual coordinate system is hop-based and unrelated to the physical location of the sensors. Thus it does not require sophisticated equipment to determine coordinates and has little overhead. The network layer also embeds an energy efficiency management module which turns off the wireless interface during periods of inactivity. These periods are computed taking into account the requirements of the network and the stream system layers.
Future work includes the study of dependable and secure communication protocols to connect the body area sensor network with domotic and hospital networks. These protocols should ensure confidentiality and protection against the transmission of malicious queries. They should ensure integration of the sensor network monitoring the patient with the medical devices and with the administrative and patient data available in the domotic and hospital networks.
Please contact:
Stefano Chessa, ISTI-CNR and University of Pisa, Italy
Tel: +39 050 3152887
E-mail: chessa![]() isti.cnr.it
isti.cnr.it

 This issue in
This issue in