This issue in pdf Subscription Archive: Next issue: July 2005 |
|
|||||||
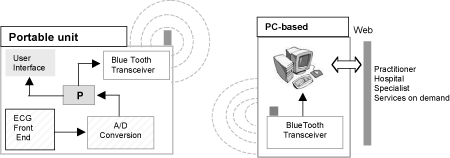
Building a Bridge for Communication between Patients, Family Doctors, and Specialistsby Matteo Paoletti, Loriano Galeotti and Carlo Marchesi According to recent reports of the World Health Organization, the next two decades will see dramatic changes in the health needs of the world's populations with chronic diseases, mental illness and injuries as the leading causes of disability. Increases in the senior population 'confined' within the home are also expected. ICT technologies must tackle this challenge by providing the means for fast communication and consulting services between the chronically ill, the general practitioner and the hospital specialist. The objective of the AMICUS project, launched in 2003 at the BIM Lab, University of Florence, is to design a personalized communication system that can improve the quality of daily life and medical care for the chronically ill, at the same time helping to reduce the number and duration of hospital recoveries. AMICUS aims at contributing to the reduction of health costs and at providing easy access to medical assistance. This is in line with a recent position statement from WHO that strongly encourages the development of devices able to give patients an active, conscious role in the management of their disease: actions are needed that emphasize collaborative goal setting, patient skill building to overcome barriers, self-monitoring, personalized feedback, and systematic links to community resources. AMICUS proposes a number of innovative solutions all aimed at increasing the control of patients over their health. First of all, patients should be encouraged to play an active role in monitoring their disease through the application of custom-designed procedures embedded in portable (possibly wearable) devices. In order to obtain the necessary medical and technical specifics for the implementation of devices of this type, AMICUS is studying the development of an instrument which will monitor the patient's vital signals and derive patterns of evolution over time. Although such devices are already potentially marketable, in our opinion a rigorous assessment phase is first needed in order to evaluate the level of knowledge and the experience necessary for a correct employment. Fully reliable systems are not yet available and a too-early introduction on the market could be dangerous. The AMICUS project will build a prototype system, known as COMPASS, which should offer wide possibilities of 'in itinere' intervention (hardware and software changes) as a result of experimentation and field trials. The system has a split architecture and consists of two units: one is a wearable Blue Tooth biosignal transmitter whose range covers the patient home area and the other is a PC work-station, which receives data from the patients and classifies events, submitting the information to the health care network, when necessary.
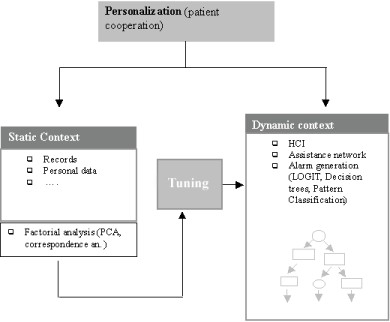
A second objective of the project is the definition of an accurate personalization of system parameters based on contextual information about the patient's case history and current dynamic conditions. A preliminary tuning is obtained on the patient's first admission, through a set of multivariate analysis techniques that indicate his/her profile (see Figure 2). This profile (or set of features) is embedded in the personalization procedure and the system's performance is then tuned accordingly.
Without the contribution of such contextual data, the signaling system would only be based on features derived from real time signals, which are usually not sufficiently reliable. On the contrary, the signals of the system can normally be correctly interpreted through human intervention. In our opinion, communication between a patient and his family doctor can be usefully supported by personal devices bridging the time interval between successive medical examinations. An additional but important feature of the system regards a set of aesthetic and ergonomic values provided by industrial designers (ISIA, Industrial Design Institute of Florence). We intend to begin experimentation of the system with a very well-defined group of patients. In this respect. we are currently talking to the Respiratory Unit of the Main Hospital in Florence with reference to the population affected by COPD (Chronic Obstructive Pulmonary Disease). On-line long-term monitoring could play an important role in the well-being of these patients. It could provide critical information for long-term assessment and preventive diagnosis for which trends over time and signal patterns are of special importance. Such trends and patterns are often ignored or scarcely identified by traditional examinations. The aim of the operational phase (data acquisition and patient profile definition) will be to produce a system prototype. During the clinical trials we hope to discover the answers to questions like: How far can we rely on cooperation from the patient? Can the patient feel confident of a timely intervention? How simple must the system be to be accepted by a typical user? How easily would it be for specialists to abandon current patient admission practice? Would such an approach be useful in reducing the number and/or the duration of hospital recoveries? Project partners:
Link: Please contact: |
|||||||